What is it like to have a Septoplasty?
I had a Septoplasty, Turbinate Reduction, and Concha Bullosa excision. I had no idea what to expect, and tons of questions before surgery. So today, I’m here to answer, in detail, the question that everyone keeps asking me, “What is it like to have a Septoplasty?”

Jump ahead to:
What were my symptoms?
Nasal Obstruction
I have always had symptoms of not being able to breathe out of my nose, but I thought that was normal. It wasn’t until I had my first baby that I noticed she slept with her mouth closed. She breathed only through her nose during naps and overnight. I couldn’t fathom how she was breathing solely through her nose. So I asked my husband if he could breathe like that too and of course, he said yes. So I started researching and asking my other family members. My research indicated that I may have a deviated septum. How did I not know this?
Sore Throat
My second symptom worsened over time through adulthood. I noticed that I frequently woke up with a sore throat. Especially in the colder months, I would wake up daily with a sore throat, but it went away after a couple of hours.
Snoring
My third symptom was snoring. Of course, I didn’t know that I snored until my husband told me.
Consecutive sinus infections
My fourth symptom was having eight sinus infections in one year.
Interrupted sleep
My fifth symptom, which became one of the worst for me was interrupted sleep. At first, I thought it was because I was a first-time mom, and not sleeping through the night became normal. But slowly, I realized I was waking up to take a deep breath through my mouth which felt like I hadn’t been breathing for a moment. I also noticed my energy levels dropped during the day from being sleep-deprived.
Headaches
And finally, my sixth symptom was when I decided enough was enough. I began waking up with headaches every day and they only got more severe. After enough research, I realized that sleep apnea can cause a person to wake up with headaches. So that’s when I called to make an appointment with the best ENT in our area. Unfortunately, because I was a new patient, I had to wait eleven months to get an appointment. So I did.
What happened at my first ent appointment?
Exam
After 11 months of patiently waiting for my new patient appointment with the best ENT doctor in our area, my appointment day arrived. I explained the numerous symptoms I was experiencing including eight sinus infections in the previous year, not breathing through my nose, snoring, sore throat, sleep apnea, and waking up with headaches. Then the ENT doctor did an exam. That’s when he told me he could see that I had a deviated septum to one side. But what was more concerning was how enlarged my turbinates were.
He proceeded to show me what turbinates were on a chart hanging on the wall. Then he used forceps to hold my nostril open and sprayed a cold spray inside each nostril a few times. He said my turbinates did not go down very much and exclaimed how they were too large for my nose. He then ordered a Head CT scan.
Head CT Scan
I went to the hospital to have a Head CT scan done. They said my doctor’s office would call me with the results. A couple of days later, my doctor called me himself and explained the results. They indicated I had a deviated septum and concha bullosa on two sides. He said a septoplasty was the only option to fix all three. So I agreed and asked him to put me on his surgery schedule as soon as possible.
Pre-surgery consultation
Insurance
I learned that in the United States, depending on the type of health insurance, some require the patient to have a pre-surgery consultation weeks before surgery. Since we were already in December, they scheduled an immediate consultation.
CT Scan and surgical plan review
At the consultation, my ENT and his nurse came in to go over the CT Scan. They showed me the deviated septum and concha bullosa. He again looked inside my nose and sprayed the cold spray in my nostrils. Once again, he said I definitely needed a turbinate reduction as well. He explained that he’d fix all three during one single surgery which would take about an hour and a half total. He said the hardest part is the first few days after surgery during recovery. The reason is that depending upon the specific type of procedure, the patient may have stitches, splints, and packing that fills the entire nostrils. His nurse said once you get through that, the hard part is over.
Afterward, his nurse proceeded to ask me health-related questions to determine if I was a high-risk surgery patient. She asked me if I drink, smoke, have any heart problems, sleep apnea, or have had reactions to anesthesia previously.
After many questions, I was given important paperwork with detailed instructions and we went over it. It included the date of the septoplasty, the address of the hospital for surgery, and if I needed Pre-Anesthesia Testing, which I did not.
very important pre-surgery paperwork
It also included the following important information about my surgery.
- DO NOT EAT OR DRINK ANYTHING AFTER MIDNIGHT THE NIGHT BEFORE YOUR SURGERY, NOT EVEN WATER!!!
- On the day of surgery, you should wear comfortable clothing. NO makeup, nail polish, jewelry, or hair clips.
- Be sure to notify your doctor if you develop a cold, sore throat, cough, fever, rash or any other illness before your surgery.
- For your protection, you will not be permitted to leave the hospital alone or drive after your surgery.
- Please make arrangements for a responsible adult to drive you home and remain with you for the first 24 hours after you leave the hospital.
- NO aspirin or ibuprofen products (Advil, Motrin, Aleve) or vitamins one week prior to surgery.
How to prepare for the day of surgery
Stop taking all vitamins and pain relievers
Since this was my first surgery, I wanted to be sure there were no blood thinners in my system. So I stopped taking all my vitamins two weeks before surgery. I made sure not to take any Advil, Motrin, or Aleve either as those thin the blood. His nurse said if I absolutely needed pain relief etc, I could take Tylenol. But personally, I didn’t want to take that risk.
On a side note, make sure you hydrate the week before surgery so getting an IV will be a lot easier.
Go ahead and purchase a new non-medicated Saline Nasal Spray to use after the packing is removed. You will also need lip balm to prevent your lips from bleeding overnight after surgery. Plus, make sure you have Tylenol. These are the ones I bought.
Arrangements for a responsible adult
We have two young children, so my husband made arrangements to take off the day of surgery, plus two days. Since he works remotely, he got permission to work nights and on the weekend to catch up on work. But it’s most important to have someone with you around the clock for the first 24 hours after surgery.
Personally, I wasn’t able to get out of bed to fix any meals or make sure I had snacks to eat for the first two days after surgery. So if you can find someone to stay with you for the first 48 hours, that would be ideal.
support pillows to sleep sitting up
Thankfully my mom decided to also take the day off for my surgery and let me borrow her wedge pillow, a couple of firm pillows, and this lower back pillow that has made all the difference in my recovery. It’s important to note that you need to sleep sitting up to reduce swelling. As long as the packing is inside your nose post-surgery, absolutely sleep sitting up.
What to wear on the day of surgery
I thought about the fact that I didn’t want anything with a small neck opening to go over my face after surgery. So I chose a stretchy shirt with a wide neck to wear under a zip-up hoodie. Since it’s winter, I also wore my coat and comfortable sweatpants. Although I wore a bra initially, I knew I would be in bed after surgery so I opted to forgo wearing a bra after surgery. This made transferring to the bed a lot easier. Thankfully, my mom helped dress me after surgery and put a scarf around my head/ears so I didn’t get an earache from the super cold weather.
Prepare your bed
I’m the type of person that loves to have clean sheets on the bed, so I made sure to wash the sheets and pillowcases and make the bed in advance. The doctor recommended having my husband sleep in a different room while I’m recovering as they’ve had situations where the spouse has accidentally elbowed the surgical patient in the nose overnight and they needed a second surgery. OUCH! So to avoid that, my husband temporarily moved into our son’s room for the time being.
Food Preparation
This final preparation has proven to be one of the most important. The day before surgery, I bought a rotisserie chicken and ingredients to make homemade chicken noodle soup. We also bought soft foods that were pre-packaged and easy to eat. Some of these foods included applesauce cups, diced peaches in natural juice, diced fruit cups, greek yogurt cups, coconut water to rehydrate, cherry juice, crackers, and bone broth.
Anti-Nausea Tip
Tip: Diced peaches in a jar or a cup with juice stops nausea and vomiting. I learned this from having two young children. So as a preventative measure, I ate a cup of diced peaches with juice along with other food before taking the pain medication and antibiotics. Because of that, I have not experienced any nausea or taken the anti-nausea medication.
What is it like to have a septoplasty? day of surgery
The morning of surgery
I stopped all food and drink before midnight the night before my septoplasty. Since my surgery was scheduled at noon, they scheduled my arrival time at the hospital for registration at 10 AM. So I set my alarm accordingly and woke up to take a shower, wash my hair, shave, and prepare myself. (You are not allowed to wear lotion, deodorant, oils, or cream on your body on the day of surgery either.)
arriving at the hospital
My husband drove me and the kids to the hospital and dropped me off at the main entrance, where my mother met me to walk in. We of course had to wear masks the hospital provided, then headed to registration. A lady at the registration desk asked for my ID and insurance card and verified my information as well as the procedure I was having that day. Then she gave me instructions for which floor to go to and handed me a file to give to the staff at the next place. My mom was allowed to go with me.
Once we arrived at the check-in for the surgical floor, I gave the lady my file and she said we could have a seat. About two minutes later, they called us back.
Hospital room and Prep
They proceeded to take us to my very own hospital room with an attached bathroom. The nurse asked me to get fully undressed and to put on the hospital gown they provided with the ties in the back. Then I placed my shoes and all the clothes I arrived wearing into a plastic bag provided by the hospital. (It’s best to leave any jewelry, valuables, cash, wallet, etc at home or have the person with you take it.) The nurse asked me if I was wearing any jewelry or had any piercings that I forgot to remove.
Once I changed into the hospital gown, they had me get into the hospital bed, change into the non-slip hospital socks, and covered me with a warm blanket. Then the nurse asked me numerous questions, verified my name and date of birth, and asked me to sign the final paperwork.
Next, a nursing assistant came in and took my vitals like temperature and blood pressure.
Then a second nurse came in to start my IV. He put the IV in my hand since that’s where I had the largest blood veins. He told me the anesthesiologist and the doctor would come in next.
Doctor visits
Once it was closer to the time of my actual procedure, my ENT doctor came in and told me that he had an emergency surgery patient being life-flighted there since they couldn’t stop the bleeding from his nose. So as a courtesy, he let me know they would be running late. I was completely fine with that. Since I have severe hypoglycemia, my ENT immediately approved a dose of dextrose through my IV to regulate my blood sugar and get me through surgery. They gave me half the dose before the surgery and planned to give me the second half after surgery.
Eventually, the anesthesiologist came in and introduced himself. Then he asked me a couple of questions and explained what the process was going to be. He said they would soon come in to give me a cocktail of medication to help me start feeling drowsy. Then once they got me into the surgical room, they would administer anesthesia with a mask and I would go to sleep.
Heading into surgery
Once it was time to head to surgery, a team of nurses plus the anesthetist came in to get me. They asked me a few questions and I said goodbye to my mom.
Then they administered the medication “cocktail” and they quickly rolled me out the door while in the hospital bed. On the way, I immediately started feeling drowsy. But I remember it all. They wheeled me into the operating room and I looked around and saw a supply closet outside the room to the left. I also saw a bunch of various nurses and doctors in the room. I looked to my right and wish I hadn’t. That’s when I saw the surgical tray lined with surgical tools and my surgeon. Finally, the anesthesiologist put a mask over my nose and said to breathe normally. I remember the mask having an off-putting plastic chemical smell. That’s the last thing I remember until I woke up inside the recovery room.
Septoplasty recovery
Recovery Room
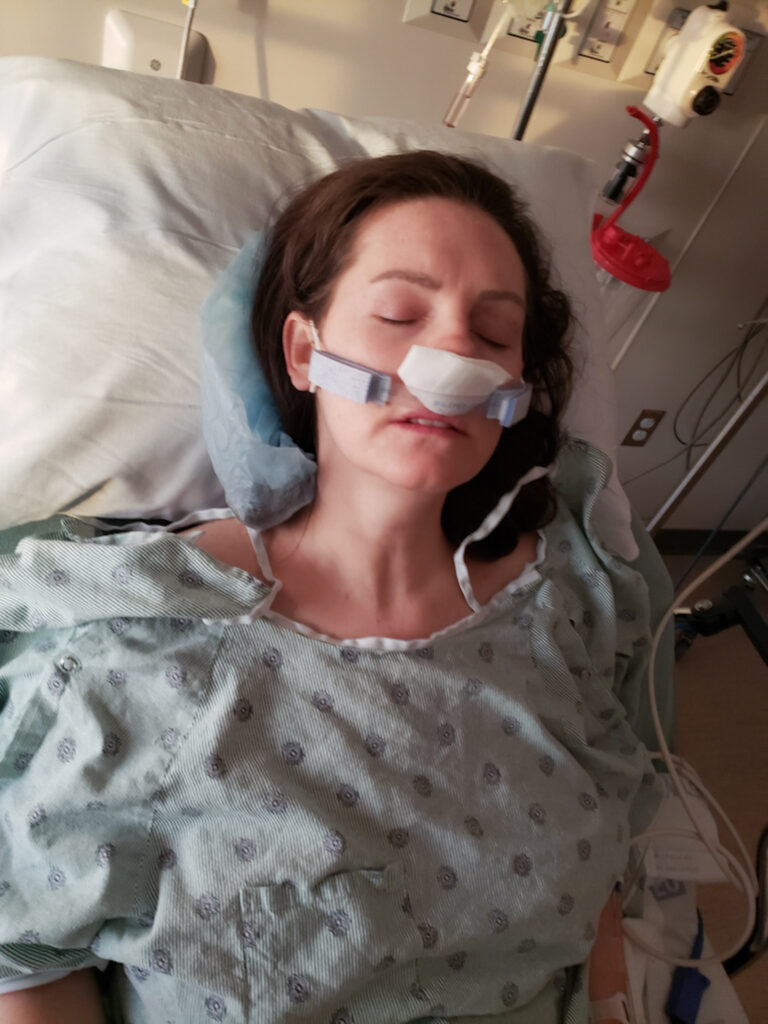
I woke up in my hospital bed with a nurse sitting next to me and felt very groggy. Once I tried to swallow, I quickly realized my mouth was dry and sore from the tube they had placed into my throat. With that pain, I couldn’t speak. I still felt tired so I was in and out of it. Finally, I opened my eyes again and tried to get the attention of my nurse. Since I couldn’t unstick my dry tongue from the side of my mouth, I tried signing to her to ask for a drink of water. She didn’t understand me plus I was still loopy so who knows what I was signing. Hahaha.
I tried repeatedly signing to my nurse to ask for a drink of water and I overheard her asking the other nurses if they knew sign language. None of them did, and of course, she told me I need to use my words. So I tried, but my words didn’t come out clearly. It’s like I couldn’t say what I needed. It was a very uncomfortable feeling to not be able to clearly communicate. She grew frustrated with me. I kept trying to say water, water, water.
Hospital room Recovery
A bit later, I woke up and I was back in my hospital room with my mother. I don’t remember how I got there. But as soon as I saw my mom, I started signing for water. She of course knows I speak baby sign language with my children and knew exactly what I was asking for. She brought me water and I motioned for her to use the straw and drop it into my mouth because I couldn’t put my lips around a cup or a straw to swallow. So she did. I’ve never felt such relief! I was able to unstick my tongue from inside my mouth and wow it was super dry!
I could also feel the pressure in my nose since it was filled with packing. Then I saw some sort of gauze under my nose because it was sticking up in the front. Finally, I felt something around my ears but didn’t know exactly what I had going on at that point. It turned out to be a nasal dressing holder.
Preparing to go home
Since my surgery started so late and recovery took me a long time, it was past closing time and the nurses were anxious to leave. I remember them being very stern with me saying I need to use my words to communicate and hurry and get dressed to leave because they were closed. I’m not sure how I got dressed or who dressed me. The next thing I remember was being wheeled through the hospital by the nursing assistant who had been rushing me. She waited with me at the entrance until my mom pulled the car around. She helped me into the car and then I woke up at the pharmacy drive-thru.

Picking up Prescriptions
I briefly remember going by the pharmacy and picking up three prescriptions. I was prescribed anti-nausea medicine, pain medicine, and an antibiotic for preventative measures.
Recovery at home
Arriving Home
We arrived home around 7 pm and I remember my husband helping me out of the car, into the house, and straight into bed. He had set up a wedge pillow, the firm pillows, and the lower back pillow in the center of the bed so I could sleep sitting up. I felt exhausted, but not in pain. I just felt pressure and stuffiness inside my nose.
Instructions, Medications, and Post-op septoplasty Review
As I lay in bed, my mom went over the post-surgical paperwork and medications with my husband. I overheard her say my ENT wanted us to call their office first thing in the morning to set up a follow-up appointment for two days after the procedure to have the packing removed. Since my procedure was late Tuesday, they requested we make an appointment for late Thursday in their office. We were told that I needed someone to drive me as no driving is allowed for the first week after surgery with the pain medication.
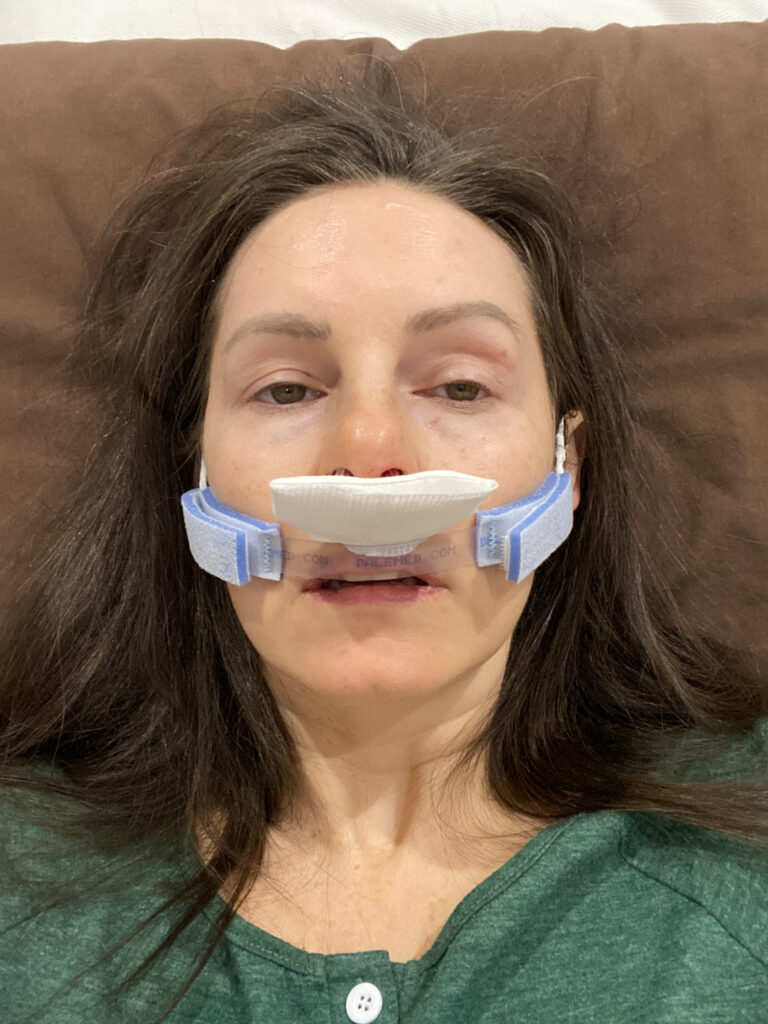
Eat
Since I had not eaten since midnight the night before, I was very hungry but I could not open my mouth very much and I felt pain in my upper teeth/jaw.
Thankfully, we had prepared ahead of time so my husband brought me a cup of soft diced peaches in juice, applesauce, broth from the chicken noodle soup, and some crackers. I quickly realized the crackers were too crunchy and I couldn’t put any pressure on my teeth or bite down to close my mouth, so I dipped the crackers in the broth to soften them. Once I had enough food in my stomach, I took my first pain pill and my antibiotic. My husband wrote down the times since the pain pill was to be administered every 4 hours and the antibiotics were every 8 hours.
Note about pain meds
Since I do not like to take medications unless I need to, the pain pill made me very drowsy. After the first two doses of pain meds, I quickly realized that they slowed my heart rate down for the first initial hour, which made me uncomfortable. So I opted to take the pain pill and make sure to stay awake for the first hour after taking it.
What is it like after septoplasty? Recovery Days 1-5
Day 1
I immediately fell asleep propped up on a wedge of pillows after taking the first pain pill and antibiotic. Of course, I was still groggy from recovery so I was in and out of it. But I made sure to wear the nasal dressing holder under my nose as I was still bleeding a tiny bit from my nose.
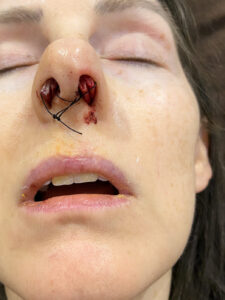
I woke up 4 hours later with a very dry mouth again and feeling the pain and pressure inside my nose, face, and teeth. I ate another cup of diced peaches in juice and yogurt. Then I took the second pain pill and fell asleep. I noticed that I kept waking up gasping for air. Because my nose was filled with packing, I could only breathe through my mouth while sleeping. That meant I slept with my mouth open which made it very dry, and still sore from the tube in my throat during surgery.
We also changed the gauze in the holder since I had some drainage from my nose while sleeping.
I did not brush my teeth this very first night because I wasn’t able to. But I did manage to carefully apply my Badger lip balm to prevent dry cracking lips. If you don’t your lips will bleed overnight.
Day 2
I woke up again 4 hours later and my sore throat was gone. I felt more like myself for the first time as the anesthesia had finally worn off. As I did, I realized that the pain medication slowed my heart rate and I had also been gasping due to sleep apneas from the gauze stuffed in my nose. I ate once again and prepared to take my second antibiotic and pain pill. My husband had to help me to the bathroom as I wasn’t quite steady on my feet yet. Then back to bed to rest. I made sure to put on my lip balm since my lips were so dry.
I began keeping track of the times I was taking the medication and noticed that I was able to go about 6 hours between pain medications instead of 4 hours. They said the first 24 hours would be the most detrimental time for the pain meds. Since I was prescribed hydrocodone with Tylenol, it helped keep the swelling down to a minimum. But I started to notice my nose was very swollen. It felt like inside as well as on the outside.
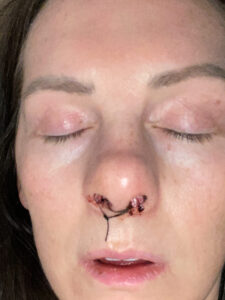
The most uncomfortable part was the packing was blocking my sinuses when I swallowed, so it allowed pressure to build up in my sinuses and my ears which was painful.
I managed to brush my teeth today. I carefully and slowly brushed my teeth but DID NOT floss. It’s too painful and risky to floss until day 5 or so.
I timed my pain medication so that I was able to take pain meds 30min. before my follow-up doctor appointment since I knew they would be removing the packing from my nose. I assumed it would be painful since I have a low pain tolerance.
Day 2 – First Follow-up septoplasty Appointment
My husband drove me to my first follow-up doctor appointment two days after surgery. I wasn’t able to wear a mask since you cannot put any pressure on your nose during this crucial healing time. I was however still wearing the nasal dressing holder in case there was any bleeding or drainage from my nose.
The nurse checked me in followed promptly by my ENT doctor that had performed the surgery.
Removing the Packing From My Nose
I sat in the exam chair and he explained that he was going to remove the packing from my nose. He adjusted my head a certain way and held it as he said to hold VERY STILL. He then used a pair of forceps to grab ahold of the packing from one nostril and he carefully pulled it partially out. Then he did the same thing with the packing on the other side. Once they were partially out, my eyes were watering. He again told me to be VERY VERY STILL and that it would be over.
Afterward, he used the forceps to grab both sides of the packing and pulled them out at the same time. I was shocked at how long they were. Attached to the end of one was a large piece of bloody mucus or a clot. It looked like a bloody snot worm to be quite frank. He closely examined it, then threw it away. I had INSTANT RELIEF! The pressure in my sinuses and ears was gone! I could actually feel the air in my nose for the first time ever and the uncomfortable pain was gone! What a relief! The nurse was right when she said the packing inside the nose was the hardest part.
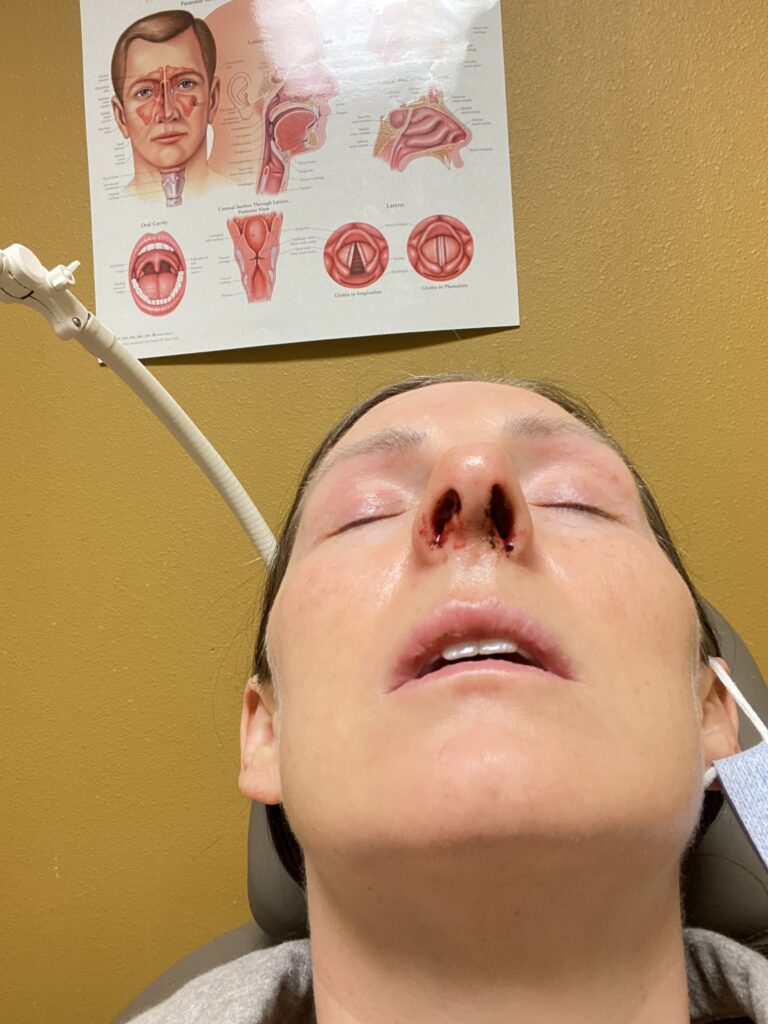
Exam
He examined the interior of my nose and explained that I have stitches on one side. I asked him how the surgery went since I was so out of it and didn’t remember much afterward. His reply was that it went well and I have small nostrils. He recommended we pick up non-medicated saline nasal spray to lightly spray inside each nostril throughout the day to keep them moist. The clarification was NOT to spray it inside my nose like a water hose but to do a very light spray and be gentle. He asked me to come back the next day because he wanted to watch for a hematoma. Finally, my husband drove us home.
Day 2 – Medication
I continued the antibiotic as prescribed and slept sitting up to reduce swelling.
I did however make the mistake of accidentally rubbing my nose in my sleep and instantly woke up in pain. As a result, I am wearing the nasal dressing holder every single night to remind myself that I just had surgery when I wake up half-asleep in the middle of the night.
Day 3 – Follow Up Doctor appointment number 2
On day three, I woke up feeling so much better and noticed that some swelling had gone down. Since the packing had relieved all the pressure, I no longer felt pain in my nose or face, so I stopped the pain meds and switched to a single Tylenol 500mg every eight hours as recommended by my doctor to keep the swelling down. I did, however, keep applying my lip balm so my dry cracked lips healed.
I continued to rest throughout the day and night and my husband brought our kids in to say good morning, hello, and goodnight before naps and bedtime. They never climbed on the bed, and I reached my hand over so they were a safe distance away to hold their hand. It’s crucial to protect your nose after surgery.
My doctor also warned me that with young children especially, it can be dangerous if they hit you in the nose. This can cause a mandatory immediate second surgery as my ENT surgeon has had to do it in the past.
My husband drove us to my appointment and my ENT said my nose looked so much better than the day before. He confirmed that I was using the plain saline nasal spray gently to keep my nostrils moist. He said to expect my turbinates to be swollen and crust over during the remaining healing process. I told him I had switched to Tylenol instead of the pain meds and he was quite surprised as most of his patients still need them at this point.
Day 4

I am feeling better day by day. The swelling is down more today, although I cannot breathe out of my nose yet due to the turbinates being swollen inside my nose. But I can now close my mouth and chew a lot easier. Finally, I finished eating the chicken noodle soup I made and crunchy crackers were no problem today.
I am continuing my 5 days of antibiotics and stopped taking Tylenol because I stopped feeling any pain.
And guess who managed to eat a big salad today without any pain or problems chewing? I did so very carefully of course.
Before bed, I very carefully took a shower. No bending, no lifting, and no straining are mandatory.
As my post-surgery paperwork explained, I used a clean q-tip and dipped it once inside peroxide. Then I gently used it to clean away any dried blood on the OUTSIDE of my nose above my lip area.
Day 5

I woke up today feeling better with less swelling. Today I noticed a new feeling inside my face. It feels almost like what I imagine having a light facelift might feel like. The best way I can describe it is like a tightness or a lifted feeling inside my inner nose area. I have continued using the saline nasal spray to keep the inside of my nose moist.
Thankfully, I’m down to the last of my antibiotic prescription as it was only a 5-day course. I usually eat greek yogurt between my antibiotics because it contains probiotics. But I plan to start my probiotics as soon as I finish my antibiotics to replenish my gut bacteria.
I am moving around a lot more, but also being very careful to not overdo it, lift, strain, or bend as required. The first week of healing is very important.
Day 6 – 21
Every single day, my nose heals a little more and the swelling goes down a bit more. Using the saline nasal spray several times a day makes a big difference. Each time I’ve had a follow-up appointment with my ENT he has said that my nose is healing very well.
By day 14 the swelling on the right side of my nose has gone down significantly and it is very noticeable. Prior to surgery, my nose stuck out a bit further on the sides of the bridge of my nose due to the enlarged turbinates. The left side is still swollen, but that is also where I have stitches inside my nose, so that’s to be expected. I am still sleeping sitting up.
On day 21, I feel significantly better and I CAN BREATHE OUT OF MY NOSE! This is the first time in my life that I’ve been able to breathe out of my nose with my mouth closed! I can’t believe it! The swelling on the left side of my nose finally went down and both sides match in size exactly. My stitches are supposed to dissolve by day 28. If not, my ENT said he will gently remove any remaining stitches on that day. I can now start lifting light things, although I can still feel it in my nose and upper teeth if I lift something.
I will continue to add updates to this post as I continue my three-week recovery. Now to answer questions I have already received.
“How painful is a deviated septum surgery?”
The surgery itself is not painful at all since you are under general anesthesia. The hardest part is the two days following surgery when the packing is inside the nose. It feels like a sinus infection, but you CANNOT blow your nose, scratch your nose, rub your nose, put pressure on your nose, or touch it during recovery. Pain medication makes a huge difference. And as soon as the packing was removed, I felt instant relief! Ultimately, I stopped taking pain medication after the packing was removed on the second day and switched to just Tylenol for the third day. By day four, I was no longer taking any medication for pain.
Rate the pain
On a pain scale of 1 to 10, I would rate this surgery a 4. I have of course given birth to two children with medication and THAT was the worst pain I’ve ever felt in my life. So deviated septum surgery was not bad at all. I would do it all over again to fix the numerous major issues I was having before this surgery.
How do you sleep after septoplasty?
You sleep sitting propped up on a wedge with a mountain of pillows and this lower back pillow to prevent back pain. You also wear a nasal dressing holder to keep the gauze under your nose. (I have continued to wear this every night during sleep to remind myself I had surgery when I wake up in the middle of the night. This has prevented me from rubbing my nose again so far.)
How long will I be off work after deviated septum surgery?
This depends on how in-depth your surgery is, how your recovery goes (if you actually take it easy), and the nature of your job.
The total recovery time is three weeks. That includes no lifting, bending, straining, blowing your nose, wiping your nose, wearing anything against your nose like a mask, and sleeping sitting upright at night. Also if you have to sneeze, you MUST sneeze with your mouth open!
If your job requires heavy lifting, then that would be dangerous for recovery and you would require more time off, a doctor’s note, and a different assignment for work while you fully recover.
But if you have a remote job or an office job, then based on my personal experience, I would have started working again on day 4 or 5 after surgery. Remember my ENT said the first week of recovery is crucial, so take it easy as much as possible.
Do they put stitches in after septoplasty?
Every surgery is different and it depends on how in-depth surgery is. In my case, I had my deviated septum fixed, a turbinate reduction, and an excision of concha bullosa, so yes, I ended up with stitches inside one side of my nose. They are dissolvable stitches and should dissolve by week four of recovery.
Is septoplasty a high-risk surgery?
Septoplasty by itself is a minor, low-risk procedure. Recovery usually takes a few days and requires an average of a week of downtime afterward. But, as with any surgery, septoplasty carries some risks, including bleeding, infection, and numbness. I experienced a bit of numbness in my upper front teeth for the first three days. That has since stopped.
Is septoplasty a major surgery?
As with any major surgery, septoplasty does carry risks, such as bleeding, infection, and an adverse reaction to the anesthetic. Other possible risks which are specific to septoplasty include having continued symptoms, such as nasal obstruction.
Shortly after the CT, my doctor called me with the results which indicated I had a major deviated septum, enlarged turbinates, and concha bullosa. He determined surgery was the best method to fix my sinus issues. Surgery was a success and now I’m here to share tips and information I wish I knew about Septoplasty, Turbinate Reduction, and Concha Bullosa removal recovery.
additional questions
If you have any additional questions, I’m happy to answer them and ask my ENT at my next appointment. Simply leave me a comment below.
If you would like to see my entire list of Septoplasty Recovery Supplies, simply click here to see them in my Amazon shop.
Disclosure: Some of the links in the post above are “affiliate links.” Therefore, if you click on a link and purchase the item, we will receive a small commission. Regardless, we give our promise that we only recommend products or services that we use personally. Above all, we believe this adds value to our readers.







Thank you so very much for your most informative article here on septoplasty surgery. I am scheduled to undergo a septoplasty and turbinate reduction procedures on March 1st, and I am most grateful for all the info and tips you have provided me. Thanks for some great writing!!
Hi Barbara! I’m so happy to hear that this info is helpful! I’ll start praying your septoplasty goes well and that you have a quick and complete recovery. It definitely helps to have support at home during recovery so if you haven’t already, this is a friendly reminder to make those arrangements if possible. You can find me on Instagram or TikTok at @TheMaternalHobbyist if you would like to stay in touch, have any questions, or update me on your septoplasty recovery. If you learn any new helpful tips, please let me know so we can help prepare others as well. Have a wonderful day!
Hello, first, thank you for your article. I am scheduled for surgery this July. My question for you is what were the results after your surgery? Did the headaches go away? I have a deviated septum and large concha Volusia on the right side of my nose, I’ve been suffering from severe head, pain and pressure for the past year. We’ve only recently found the contra Bluejay and hope that the correction to it and the septum will bring relief from my head pain. I noticed in your article that headaches are one of the last symptoms to form so I’m curious where your left now after having surgery and if it was worth it?
Hi, I am now 7 months post surgery and I wish I would have had the surgery much sooner! I can sleep without waking up gasping. All my symptoms have completely stopped. I can actually breathe with my mouth closed. I’ve never been able to do that, so this surgery has been life changing. I finally feel well rested after sleeping and I wake up on my own after less sleep, which is new. It was 100 percent worth it! Finding a reputable surgeon is the most important part. I’m so glad that relief is soon for you!
Hi, I had the same surgery. They gave me anesthesia. And I think because of that I started having issues with my bladder. I had a urine retention in my bladder which was painful. Did you had similar bladder issues and how long it took to recover
Hi Viraj, I’m so sorry you’re having trouble since your procedure! I will say, I had a previous procedure that involved me needing a catheter, and because of that, the catheter caused scar tissue inside the urethra and my bladder started retaining urine and I had non-stop UTI’s. I went through 18 rounds of antibiotics in a year until I found a new doctor who said we should do a Cystoscopy to look at the urethra and the bladder. However, he couldn’t get the scope in. His nurse assisted and said that the scar tissue had almost completely closed off my urethra so the urine was not able to completely drain from my bladder. They ended up stretching out the urethra and had me use the bathroom. It worked! I was able to go to the bathroom immediately without a problem and I stopped having UTI’s from that point on. If I do feel a UTI coming on, I take a cranberry supplement and drink lots of water throughout the day to clear out any bacteria in the urine. Please see a Urologist and let them know that since you had the procedure with a catheter, you’ve had issues and ask them if they will consider a Cystoscopy to look and find the cause of the issue. Since the cystoscopy I was told to always request a pediatric catheter if I ever need a procedure. That will prevent damage to the urethra that can cause scar tissue to develop. Please let me know how it goes and I’m praying for your complete recovery!
Hiya, could you put more before and after pics? Does it change your nose shape?….I cant breath and I really want this surgery but, I’m a bit worried about the shape after
Hi, I’m happy to send you more before and after photos. Are you on social media somewhere so I can direct message you and answer any other questions you have? I’m on Instagram and Facebook and TikTok as @TheMaternalHobbyist if you would like to message me directly.
Hi Misty!
I’m so happy for you that everything went well and your symptoms are gone! That’s what I call a successful surgery! I appreciate your detailed account of what you did pre and post procedure. I recently had a surgery and you did a great job explaining the everything- very informative and helpful! In my recovery for a 90 minute surgery I had the worst taste in my mouth from the anesthesia. I had read that having mints help with the taste, dry mouth and even help with “waking up” your intestines. I had post op nausea and the nurse gave me an alcohol wipe to smell- and it worked! It’s amazing how our bodies can recover from experiences like this. You were a very good patient and I’m so happy that you had such a good outcome. Rest is so important! As is following the instructions.
Again, thanks for sharing your story! Here’s to great sleep and easy breathing! 💕
I found this looking for info on my upcoming septoplasty.
I have a severe deviated septum and according to my CT, 3 out of 4 oh my sinuses are blocked.
Like you, I can’t breathe through my nose with my mouth closed. Mine is so bad, I can’t blow air out through my nose when underwater swimming! So I am so looking forward to it.
Thank you so so much for your detailed pre-op and post-op experience.
I feel very well armed with info and am going on to my surgery full knowledge of what to expect. ❤️
Hi Heather! I’m so happy to hear that this information is helpful! I couldn’t find any information like this before my surgery which is why I wrote about it. I’m not sure when your procedure is, but I’ll be praying for you and your recovery. Make sure to have someone drive you to your post-op appointments. Once you get the packing out, you will feel so much better! I’d love to hear how you’re doing after your surgery and recovery. Plus, if you have anything to add to this experience, it can help other people.
This was so helpful! I have been in sinus infection purgatory for a long time now w constant reoccurring ones. I just scheduled my surgery today – and it’s one month before we take our two kiddos to Disney! Appreciate your details and tips, and I’ll be ordering the pillow and lip balm.
Do you think Disney 26 days later is do able? Did you have any bruising under your eyes?
Also beautiful family! What’s your Instagram?!
I’m so glad this info is helpful! I’m sure you will be so glad to stop having those sinus infections. I think Disney a month after surgery is doable as long as make all your follow-up appointments and your doctor clears you to fly. Thankfully, I did not have any bruising under my eyes. They did not have to break my nose to reset or anything so it was a bit more gentle to for them to simply remove the cartilage and repair the septum. Thank you so much for the compliment! I am @TheMaternalHobbyist on Instagram. I also linked all my social media at the top of my blog on the desktop version. I’ll be praying for you, your surgeons and your surgery and recovery mama! – Sincerely, Misty
Hi Misty!
I have my surgery tomorrow and I’m shitting bricks as this is my first surgery in the 35 years of my life.
I can’t tell you how much your detailed experience helps. I cannot wait to breathe properly and wake up without a headache or go about my day without any pressure built up.
Thank you !
Hi! I’m praying that your surgery went well! I know it can be pretty scary to have surgery, especially a surgery like this on your face. I was in the same situation and I was pretty nervous. However, the results and being able to breathe properly is definitely worth it. I know you’re still within the first couple days with the gauze still inside your nose and that’s the hardest part. I hope to hear back from you once you fully recover and see how you’re doing. I’m also interested to know if your experience was similar to mine or if there is any helpful info we can add for other people in this same situation. – Sincerely, Misty
Great to read this article! I see in the recovery portion that there should be no pressure on your nose, so I am wondering about eyeglasses? I’m pretty blind without them can people wear eyeglasses after septoplasty turbine reduction?
Hi Deb, My doctor specifically told me not to wear sunglasses to avoid pressure on the bridge of my nose. He did say up high was okay if I needed to, but DO NOT let them be lower on the bridge of the nose. I would definitely ask your doctor since you need to wear eyeglasses to see. I’m sure your doctor will have experience with that. I would love to know what he/she says in case anyone else has this question too.
Writing from India: Thank you for putting this up.
I relate to so many of your “before” symptoms, and I’m prepping for the procedure in the coming week.
I think I got more info here from the doctor’s office. Glad I found this piece.
Hi Arnold! I hope your procedure went well! How are you feeling? Has you recovery been similar to mine?
Did the shape of your nose change?
It did surprisingly! It looks smaller and the bulbous tip is no longer bulbous. It looks SO much better and I had no idea that would be a perk of this procedure. I would do it all over again.
I just had the septoplasty this week and I feel like my nostrils look off. Did you find this to be true while you had stints in and swelling that your nostrils looked off from one another.
Hi Hiliary, Yes, nothing looked normal for a while after surgery. There is so much swelling that it takes a long time for all of that to go down before your nose starts to look somewhat normal. I noticed that my nose was STILL healing even 6 months after my septoplasty. So not to worry. It definitely takes time for the body to heal all the different parts inside and outside the nose as well as for the swelling to decrease. Doing the saline daily and following the after care actually allowed for a more speedy recovery. My ENT said he had never seen anyone else’s nose heal that quickly. I followed the after care protocol EXACTLY. Hope this helps! Feel free to reach out with any further questions!
Thank you for the detailed article. I am surprised your doctor didn’t send in the prescriptions on the day of the preop appt. Prescribing them on the day of the surgery is not standard practice. If you had to use a medical transport company instead of a family member they would have charged you for a stop. I have had 15 surgeries in the last 30 years and never seen this. An ultrasonic humidifier with heat can really help with the sore throat while mouth breathing during healing. I am happy you finally have the way overdue relief! My best, Stacy
This was my first surgery, so I didn’t know that sending the prescriptions on the day of the surgery isn’t standard practice. Thank you for that information! I actually haven’t heard of medical transport either. Excellent tip with the ultrasonic humidifier! Thank you so much Stacy!
Thank you for an excellent written description. It made me know what to do and get. Also, I heard sore throat spray is good for tubing in throat. Helps with soreness of throat.
Sore throat spray is such a great tip! Thank you for adding this tip! Have you had your procedure yet? If so, how is recovery going?
Thank you for sharing this! I’m on day two post-op for septoplasty and turbinate reduction and I was not prepared for the amount of swelling and discomfort. Your day to day breakdown gives me hope though. I get my interior splint removed Monday and am hoping that provides some relief
How are you feeling now? I hope you’re doing well!